Swallowing is something most of us don’t think about until it becomes uncomfortable, stressful, or even scary. If you or someone you love has started coughing during meals, avoiding certain foods, or feeling like food gets stuck, you’re not alone. Swallowing difficulties are known clinically as dysphagia, and they can affect adults for many reasons, from neurological changes to reflux irritation or recovery after illness.
The good news is that dysphagia is treatable, and help is often more straightforward than people expect. With the right evaluation and therapy plan, many adults improve comfort, confidence, and safety while eating and drinking.
If you’re in Toms River, NJ, or nearby Ocean County communities, Shore Therapy Services can help you take the next step with a compassionate, practical approach, so meals feel calmer again.
Common Signs of Swallowing Problems in Adults
Swallowing challenges don’t always look dramatic. Sometimes they show up as subtle changes you work around without realizing it.
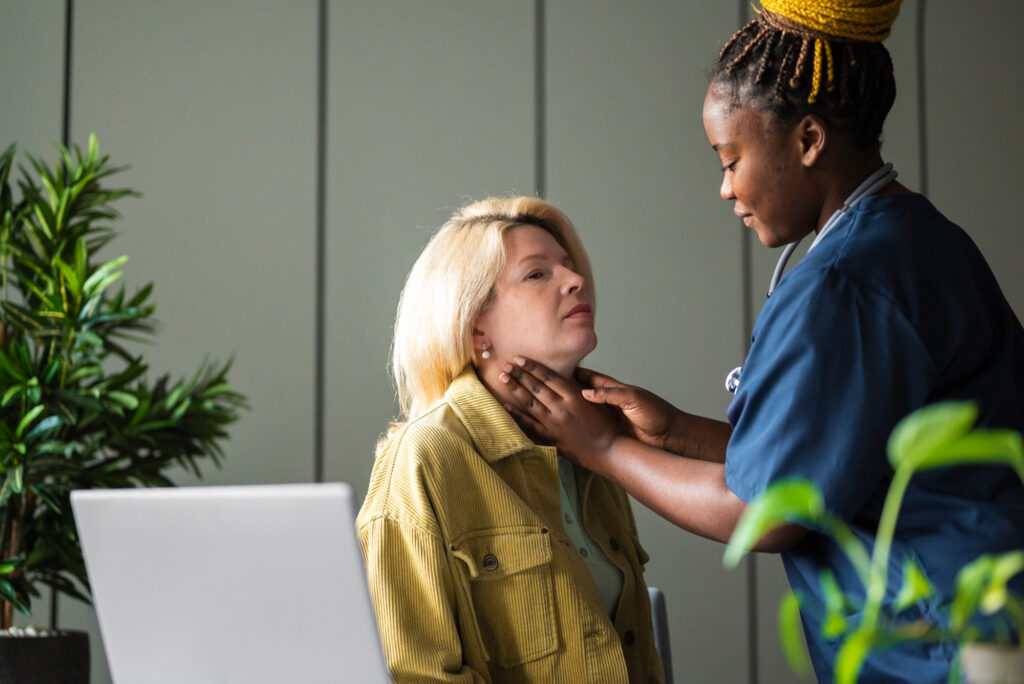
Here are common signs families report:
Signs that show up during meals
- Coughing or choking while eating or drinking
- Frequent throat clearing during meals
- Trouble starting a swallow, or needing multiple swallows per bite
- Feeling like food is sticking in the throat
Signs that show up right after swallowing
- A wet or gurgly sounding voice after eating or drinking
- A sensation of residue left behind, like you need to swallow again
- Shortness of breath or fatigue while eating
Signs that show up in everyday habits
- Avoiding certain textures, such as crumbly foods, dry meats, or thin liquids
- Taking much longer to finish meals
- Eating less in social settings due to worry or embarrassment
- Unplanned weight loss, dehydration concerns, or reduced appetite
- Recurring chest infections can be associated with aspiration risk in some cases
When to treat symptoms as urgent
If someone has sudden, severe difficulty swallowing, drooling they can’t control, new facial droop, severe weakness, confusion, or breathing distress, seek emergency medical care.

For ongoing, non-sudden issues, scheduling a swallowing evaluation is often the right next step.
Why Dysphagia Happens in Adults
Swallowing is a coordinated process involving the brain, nerves, muscles, sensation, and breathing. When any piece of that system changes, swallowing can change too.
Neurological changes
Dysphagia is especially common after stroke and can also occur with conditions like Parkinson’s disease or other neurological diagnoses.
Medical, structural, and recovery-related factors
Adults can experience swallowing changes after:
- Surgery or medical procedures
- Head and neck treatment and recovery, depending on diagnosis and care team
- Reflux or irritation that affects throat comfort and sensation
Breathing and swallow coordination
Swallowing and breathing are carefully timed. When breathing is compromised or coordination shifts, people may cough or feel out of sync during meals.
What a Swallowing Evaluation May Look Like
One of the biggest barriers to getting help is not knowing what will happen in an evaluation.

A supportive swallowing evaluation is focused on clarity, comfort, and practical next steps.
Step 1: A conversation that matters
Your clinician will ask about:
- What feels difficult, including solids, liquids, pills, and specific textures
- When it happens, such as first bites, later in meals, or only when tired
- Medical history that may be relevant
- Your goals, such as eating out again, drinking water comfortably, or reducing coughing
Step 2: A clinical assessment
A clinician may observe factors related to swallowing function, such as oral control, voice quality, breathing, and safe trial strategies when appropriate.
Step 3: When additional testing may be recommended
Sometimes a clinician may recommend additional medical testing through the appropriate medical channels to better understand what’s happening and guide the safest plan.
What you should leave with
A good evaluation should end with:
- A clear summary of what’s most likely happening
- Specific strategies you can start right away
- A therapy plan with measurable goals
- Guidance on next steps if collaboration with medical partners is recommended
How Swallowing Therapy Helps Adults
Swallowing therapy is not one size fits all. It’s personalized to your symptoms, medical picture, and daily routine, with the goal of helping you eat and drink more safely and comfortably.

Strategies for safer swallowing
Therapy may include practical adjustments such as:
- Pacing, which means slowing down without feeling restricted
- Small changes in bite size, sip size, or alternating bites and sips
- Posture and positioning strategies that support safer swallowing
- Environmental changes, such as less distraction and better mealtime setup
Skill building and exercise, when appropriate
For some adults, therapy may include targeted exercises to support strength, range of motion, endurance, and coordination.
Texture and consistency guidance
If certain foods or liquids trigger symptoms, a clinician may guide you toward safer options in a way that still feels realistic and satisfying, because quality of life matters.
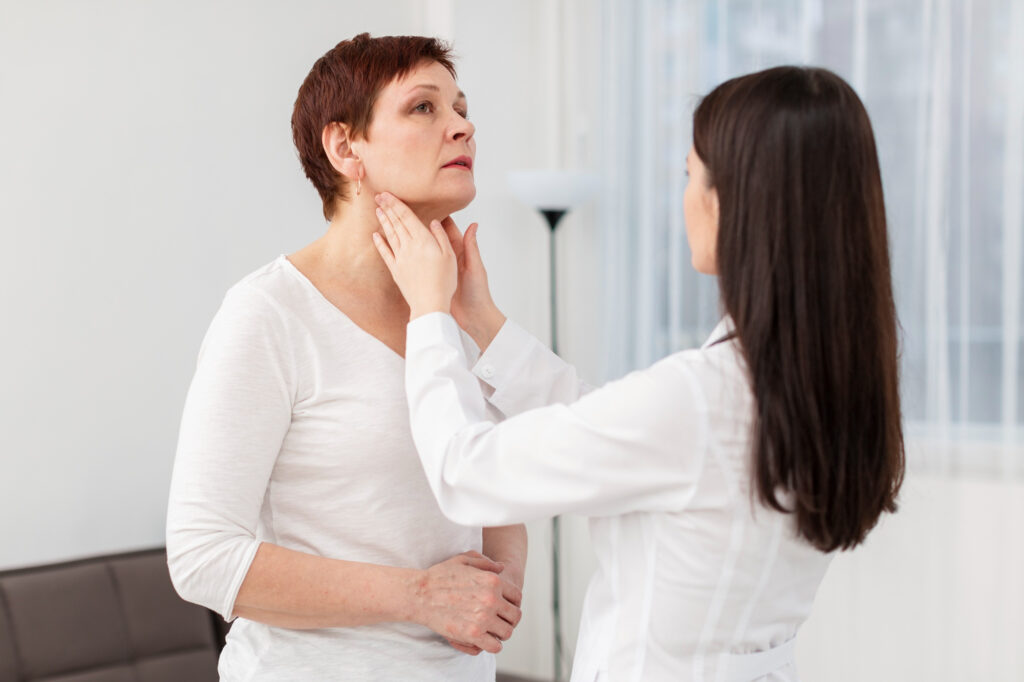
Family and caregiver support
For spouses, adult children, or caregivers, the right guidance can reduce anxiety and guesswork. Therapy can include simple cues and support strategies without turning meals into a stressful performance.
What Progress Can Look Like
Progress often comes as a series of practical wins:
- Less coughing and throat clearing during meals
- More confidence drinking water or eating in public
- Reduced fear and avoidance of certain foods
- Better hydration and nutrition routines
- More comfortable, calmer mealtimes
If dysphagia is related to a medical event, like stroke, early screening and treatment planning are often important for reducing complications.

Helpful Tips Before Your Appointment
These aren’t a substitute for an evaluation, but they can make your first visit more productive:
- Keep a simple symptom log for three to five days, including what you ate or drank, what happened, and when symptoms occurred.
- Note patterns. Is it worse with thin liquids, dry foods, or when you’re tired?
- Bring a medication list and relevant medical history.
- Don’t push through frequent coughing or choking. It’s a sign your swallowing system may need support.
When to Schedule a Swallowing Therapy Appointment in Toms River
Consider booking an evaluation if you or a loved one has:
- Ongoing coughing or choking during meals
- Food sticking, frequent throat clearing, or a wet or gurgly voice after swallowing
- Avoidance of certain foods or fear around eating
- Swallowing changes after stroke, illness, surgery, or neurological changes
Warm next step
If you’re local to Toms River or Ocean County, Shore Therapy Services can help you understand what’s happening and build a plan that supports safer, more confident eating and drinking. Contact Shore Therapy Services to schedule an appointment, and feel free to bring a spouse, partner, or caregiver if that support is helpful.
FAQs
What is dysphagia?
Dysphagia is the clinical term for difficulty swallowing. It can involve trouble with solids, liquids, or pills, and may show up as coughing, food sticking, or voice changes after swallowing.
Is coughing when I drink water a red flag?
Frequent coughing with liquids can be a sign your swallowing system needs support. It’s worth scheduling an evaluation so you don’t have to guess.
Can reflux cause swallowing problems?
Reflux can irritate the throat and contribute to uncomfortable swallowing sensations for some people. An evaluation helps clarify what’s most likely going on and what will help.
Do I need a referral for swallowing therapy in New Jersey?
Some swallowing services may require a referral depending on the situation. Shore Therapy Services can tell you what’s needed when you call to schedule.
How long does swallowing therapy take?
It depends on the cause, severity, and your goals. Many adults start with an evaluation and a short, focused plan, then adjust based on progress and comfort.
What should I bring to my first appointment?
Bring a medication list, relevant medical history, and your symptom notes, including what’s hard, when it happens, and which foods or liquids trigger it.
